When Gary Chefetz, head of MSProjectExperts, moved to Coachella Valley in Southern California’s Riverside County, he sought to give back to his new community in a way that had a “much higher impact” than simply serving soup in a kitchen. His physician, with whom he maintains a “strong relationship,” told Chefetz that he and others had coalesced a group of MDs representing a broad cross section of health care providers in the valley, all interested in pursuing Patient Centered Outcomes Research (PCOR).
The doctor, Richard Loftus, brought Chefetz in specifically to help the fledging group create a website. As it turns out, there was a whole lot more Chefetz was able to bring to the project.
Some Background
The region, home of Palm Springs, Rancho Mirage and other small towns, possesses a unique demographic. Of the nearly 435,000 people who live in nine cities and various unincorporated communities, a large percentage is aged 65 or older (19 percent vs. 10 percent for the entire county), and a disproportionately large number self-report as LGBT. The combination of those two elements makes for a unique dynamic: Many residents have lived with HIV or AIDS for decades.
For example, the average age of people living with HIV in Coachella Valley is 51 years, compared to 40 in the rest of the county. Nearly a quarter (24 percent) of those living with HIV are 60 or older; in the rest of the county only 7.5 percent of those with HIV are over 60. Among people living with AIDS, 29 percent in the valley are 60 or older compared to 16 percent in the rest of the county.
HIV was identified more than three decades ago. Highly active antiretroviral therapy (HAART), an ever-evolving set of customized medicines, has been in use since 1996, changing what was once considered a fatal diagnosis into a “chronically managed disease,” as the National Institutes of Health report. People who might have died years ago have become long-time survivors.
“It’s the graying of the HIV epidemic here in the United States,” notes Chefetz. “We believe that more than 50 percent of the people living with HIV/AIDS are 50 or older.”
What researchers understand about HIV and aging is evolving with the epidemic. The goal is to leverage the distinctive population of Coachella Valley to study HIV and AIDS and aging in order to improve the outcomes of treatments physicians and other care providers can deliver to their patients.
Obstacles and Opportunities
The research project wasn’t without obstacles.
Chefetz’s new home is the second most medically underserved region in the state. The closest clinical research centers are more than a hundred miles away in Los Angeles, San Diego and Orange County. Plus, there’s no significant academic presence in the valley.
A larger issue was this: commercial clinical research “doesn’t like to include old people,” he says. “There are too many confounding problems.” That makes for a “paucity” of research that includes older populations, he adds.
However, there are also opportunities that the organizing group wanted to exploit. First, there’s that “unusual population concentration” of middle aged and older people living with the disease
Also, one of two local hospitals recently added a residency program and the other is working on one. Younger doctors, noted Chefetz, “light up” at the prospect of being involved in research. There’s also “unprecedented” cooperation between healthcare providers at the grassroots level.
The Affordable Care Act mandates PCOR, putting an emphasis on measurement and reporting of quality outcomes (with the eventual intent of linking payments to quality outcomes). That’s precisely what the Coachella Valley Community Research Initiative is intended to produce: better outcomes for patients based on the sharing of data related to what’s working or not.
“This type of research is very performance driven. You can look at its standards like strategic drivers for improving healthcare,” Chefetz insists. “The more aligned with these values the research is, the more likely it is to produce the expected results — to improve the patient outcomes. People will live longer or they’ll live with less pain, or they’ll live with less disability or impairment. And [they’ll have fewer] bad effects from aging.”
Near-instant Infrastructure
Chefetz’s initial foray into the project occurred during a focus group that Loftus had convened to get patient input. From there, Chefetz attended a potluck at which he learned more about “Geriatric Research of AIDS Comorbidities in the Inland Empire,” otherwise known as “Project GRACIE.”
At that point the project was a shared vision among local doctors and other healthcare stakeholders. “There was no elevator pitch. This was a deep burning desire to do research, because they have all these aging patients for whom they want to provide better outcomes,” Chefetz explains.
The word to the community was that Project GRACIE would be a 10-year longitudinal study to collect data as the “face of HIV” evolves. “The people who are getting HIV now and getting early suppression, those people haven’t come of age yet,” Chefetz says. “We’re going to have to play this out for 10 years to be able to keep the results relevant, because we expect them to shift.”
Chefetz drew in part on his experience implementing Microsoft Project Server in the pharmaceutical and biotechnology industries, not as a science subject matter expert, but as somebody with start-up skills and relevant process knowledge and experience. He knew what had to be done to get the project off the ground.
So that’s what he did.
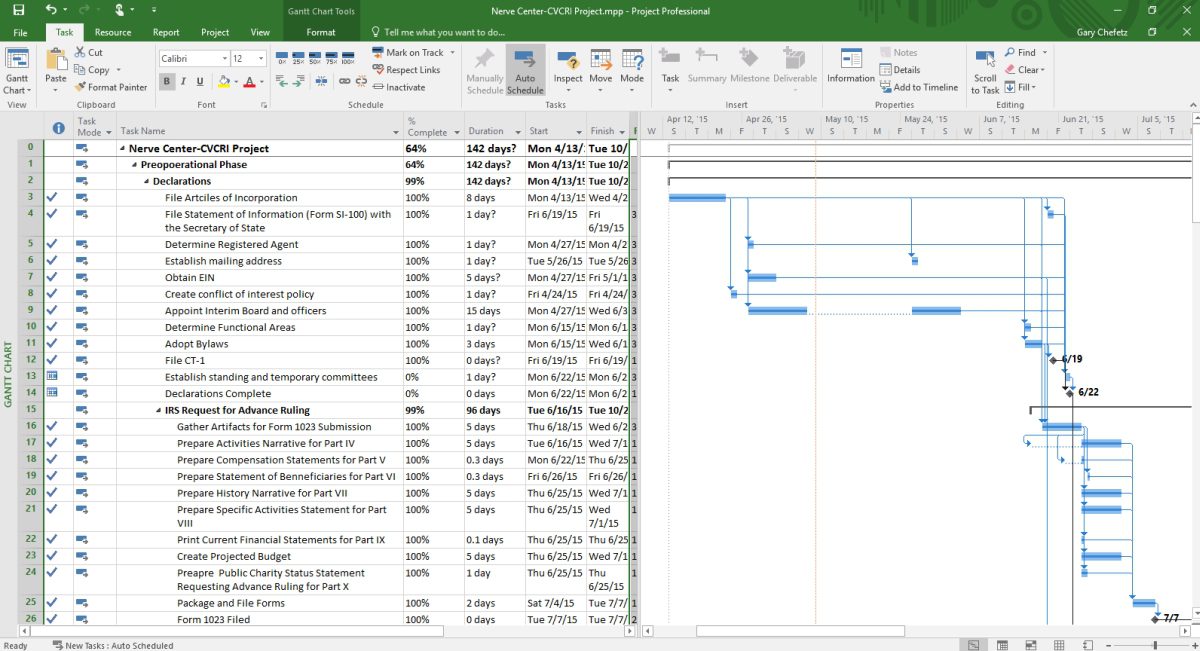
First up, creating a roadmap in Microsoft Project to get through the first phase of the project, enabling the fledgling organization to start asking for money. “Until we could offer a tax deduction,” he says, “we didn’t know if it was worth doing.”
Ninety days after that potluck, Project GRACIE’s parent organization, the Coachella Valley Community Research Initiative (CvCRI) had incorporated, had a logo, had a website, and Chefetz had implemented a financial system as well as an Office 365 portal for cross-collaboration. “Our IRS filing was complete, and at that point we’d spent less than $300 on technology,” he notes.
The technical underpinnings were completely cloud-based. “The type of organization we’re building operates in a virtual plain. It’s nobody’s primary place of work,” Chefetz explains. “The less infrastructure we have, the better — the more money can go into the research.”
He adds that project management is different when your resources are volunteer rather than paid. “The concept of schedule is more advisory. The difference between baseline and actual is the difference between what could happen if you paid people to do the work versus what happens when you have to wait for volunteers to complete critical tasks.”
Make a Difference
Progress on Project GRACIE continues apace. Chefetz says the organization is negotiating a possible partnership with the University of California Riverside Medical School. The first major fundraiser is being scheduled to take place at Sunnylands, the West coast “Camp David,” an historic retreat for world leaders. And grant money from pharma and foundations is being pursued. CvCRI is also developing its registry protocol, which lays out the details and rules about how research will be managed.
“We have unusual talent assembled,” Chefetz muses. “The next challenge we face is, how do we create a governance structure that interfaces across healthcare providers, our organization and our [future] academic partners?”
The approach of CvCRI is new, but the impact could be big. “We’re going to bring together a community advisory, healthcare providers and other important stakeholders in a new way that could address improving healthcare regionally. Ultimately, what we’re building could be a model to duplicate in other places. If we can make it work here, why can’t they do it in other areas?”
Chefetz acknowledges that he has a stake in the outcome. “That’s my secret goal — to live longer and help other people live longer.”
But there’s also something satisfying, he refrains from saying, in bringing qualities to the job that not everybody possesses. As he advises, “Realize the value of your skills and how they can easily translate into charitable and do-good endeavors. Use your skills to make a difference not only in your career but in your community.”
Image courtesy of Hoffnugsschimmer — CC 2.0